In 1963, Leon Goldman became the first person to report using lasers in dermatology. Goldman reported the effects of Ruby laser in the selective destruction of cutaneous pigmented structures, like black hairs. Since then, lasers have been used for various skin treatments such as vascular lesions and cosmetic surgery. Studying laser tissue interactions is crucial for making advances in new treatments.
Depending on the application, such as removing skin tattoos or stimulating the dermis, various laser choices exist. For example, high energy CO2 lasers can be used to remove tattoos, whereas Nd:YAG and diode lasers can be used to stimulate the dermis. Knowing the biological factors that are at play in laser tissue interactions can help practitioners choose their lasers carefully.
In this article we will discuss the factors that influence laser interactions with skin such as penetration depth, absorption chromophores, and ablation profiles. The use of various diode lasers for targeting chromophores are also discussed. The specific applications of lasers in tattoo removal, and other dermatological applications can be found in other FindLight blog articles.
Skin Profile
The human skin has the epidermis which is about 100 um thick, with the dermis extending to 1.6 to 1.9 mm. The depth is not the only anatomical factor that makes penetration hard. One must also consider the distribution of light absorbing molecules such as chromophores in different layers. This can vary for different people, which makes uneven delivery of laser energy for different skin profiles. Nevertheless, treatment has still been found to be effective for surface skin treatments, with care to be taken for monitoring deep skin treatments.
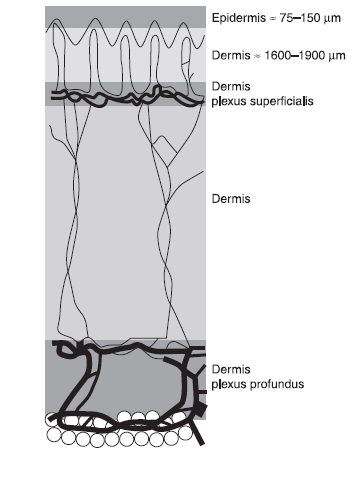
Relative depth of various layers in human skin.
Laser Tissue Interaction
Laser tissue interactions can be classified into four types on contact: reflection, absorption, scattering, and transmission. Reflection wastes laser energy and makes it unsuitable for medical applications. Absorption at the surface is influenced by various chromophores as we will in detail later in this article. Transmission helps the beam to penetrate the surface tissue to reach layers underneath. For example, choosing visible light instead of UV helps light penetrate the cornea, lens, and image the retinal layer. Finally scattering opposes precise delivery of the laser energy to a spot. In this blog post we will focus on absorption profiles and transmission depths, as these are the main forms of laser tissue interactions.
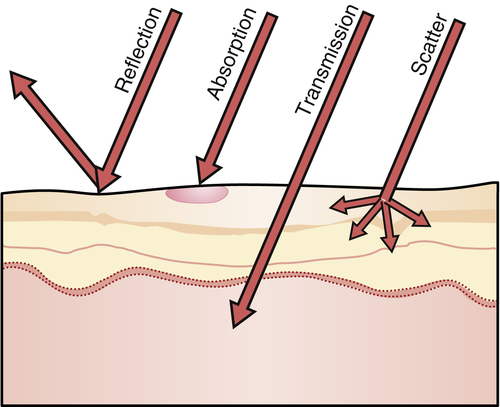
Laser tissue surface interactions. Image courtesy of pocketdentistry.
Absorbing Chromophores
Absorption in tissues occurs because of certain molecules that absorb strongly at a particular wavelength. Specifically, melanin, hemoglobin and water are the main molecules that absorb light in the skin. The absorption profiles for these molecules are shown in the image below. Consequently, this can be a useful guide in choosing a laser wavelength based on the molecular content of the tissue.
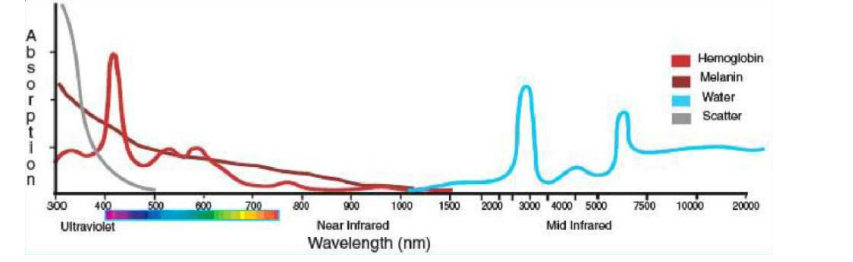
Absorption strength of various chromophores in biological tissue. Image courtesy of Optics&Photonics.
Absorption Zones
Apart from the absorption wavelength, the profile of surrounding tissue affected is important to achieve precise effects. The following diagram shows the various zones of affected tissue at the region of laser application.
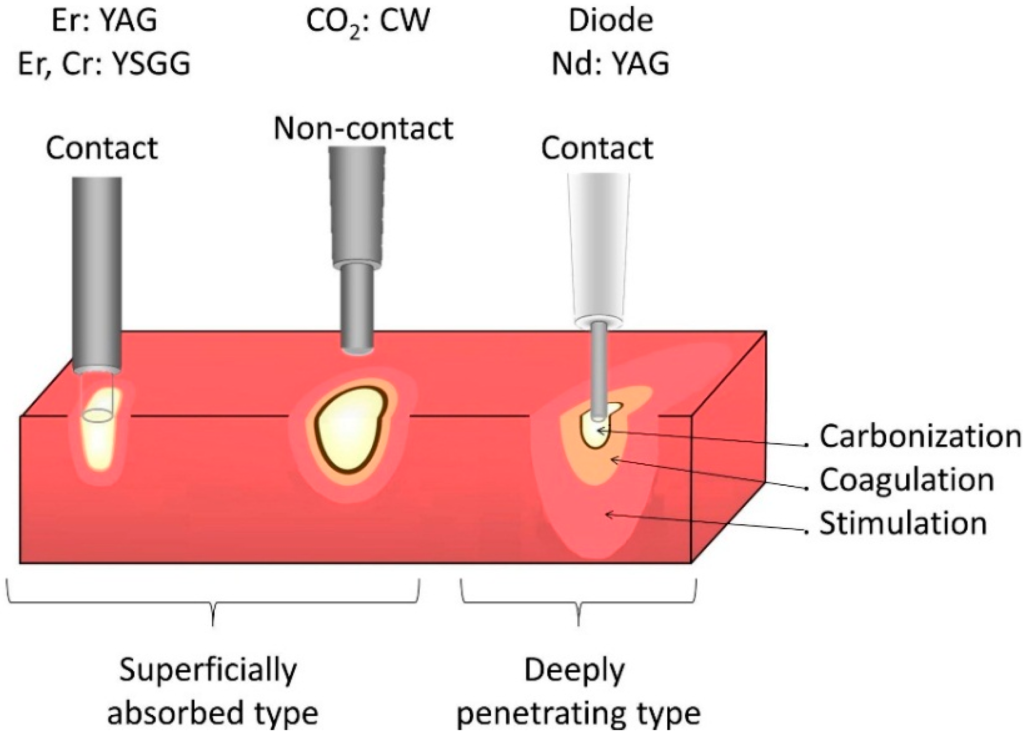
Absorption zones depending on contact and pressure for various lasers. Image courtesy of ResearchGate.
The contact tip, pressure, pulse energy and beam profile all play a significant role in this process. Applying pressure with the contact can achieve photoablation effects as shown in the right. On the other hand, a flat beam profile removes a flat tissue region. If a non-flat beam is used, then the profile of the beam influences the profile of tissue ablated. The laser beam profile can meticulously be monitored using beam profilers. The pulse energy and mode of operation (pulsed or CW) can determine whether the application is for heating or ablating a tissue. Moreover, using small pulses can reduce the thermal conduction to surrounding tissues.
The profile of the tip can also influence the surrounding regions affected. The contours of heat conduction is shown in the image below.
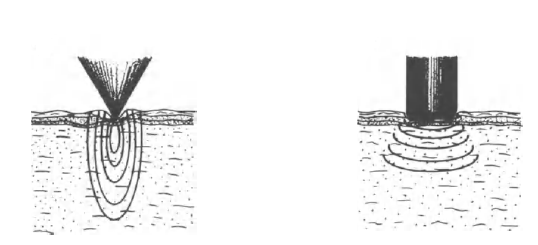
Tip geometry and contact pressure influencing energy distribution.
For pointed tips, the conduction is elliptical, and reaches a higher depth. Flat tips conduct in concentric circles. The depth and the ablation profile determine the type of tip used.
Penetration Depth
Wavelength choice plays a crucial role in the penetration depth of laser light. As shown in the diagram below, wavelengths close to red penetrate the deepest, and light close to UV remain within the epidermis.
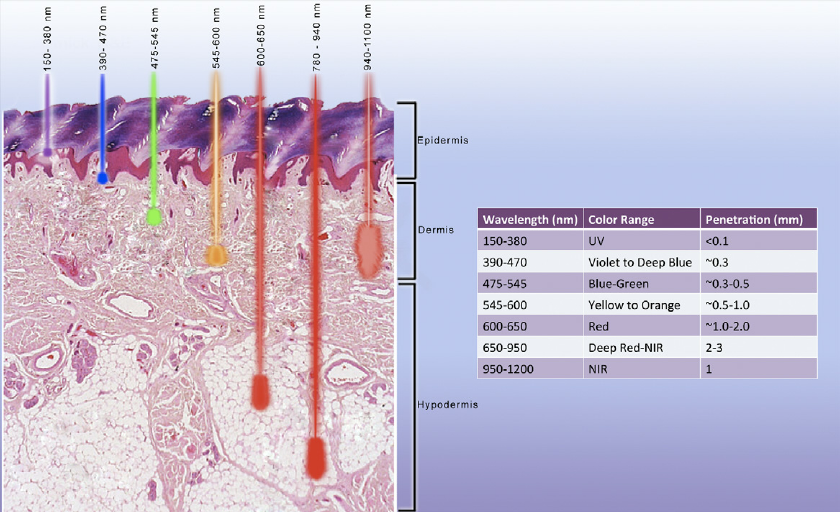
Laser tissue penetration depths for various wavelengths. Image courtesy of ResearchGate.
Shorter wavelengths are preferred for applications limited to the epidermis, while near red wavelengths are optimal for dermal applications. Nd:YAG and diode lasers exist for near red spectrum, which makes them more suitable than CO2 lasers for deep skin applications.
Diode Lasers in Dermatology
Diode lasers can emit wavelengths in the visible and infrared region. One can use a specific diode laser depending on whether the intended absorbing molecule is hemoglobin, melanin, or water. For example in blood flow measurements of blood vessels close to the surface, a technique called Laser Doppler Flowmetry (LDS) is used. This can be a useful technique in dermatology to learn about the blood flow close to the skin surface. In this technique, the light reflected from hemoglobin molecule is used to detect the velocity of the red blood cells. Since hemoglobin reflects red strongly, diode lasers with emitting red light can be used in LDS.
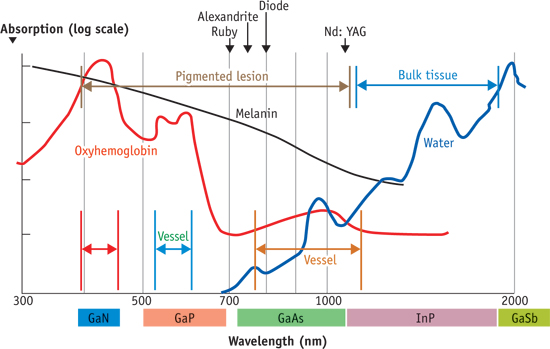
Diode lasers for various wavelengths vs the absorption profiles of various chromophores. Image courtesy of BioOpticsWorld.
Diode lasers are becoming more popular in dermatological applications because of higher penetration depth, low cost, and compact size. Check out FindLight’s collection of diode lasers to use in your projects.
