Adaptive optics is a technology to compensate for distortions in an imaging system. It typically uses a deformable mirror, that deforms to adjust for incoming distortion as the image is taken. It has been especially useful in ophthalmology when paired with a wavefront sensor that detects interference from the eye. This technique applies well to a scanning laser ophthalmoscope. Without adaptive optics and wavefront sensing, scanning lasers would be unable to render a clear image from a moving eye.
With an adjustment for interference, adaptive optics scanning laser ophthalmoscopes produce a detailed, live view of the retina. These are indispensable tools in modern ophthalmology as many eye disorders stem from the retina and need in-depth imaging. These include age related vision loss and glaucoma.
The dimensions required to integrate both adaptive optics and wavefront sensors are rather large making these ophthalmology tools an immobile furniture. As a result it forces the patient to sit upright for several minutes as the scanner operates. Even then, the image gets disrupted by minor eye movements, so the patient must be totally still. Optical CT scans are becoming a popular alternative but are invasive in their own right. In this OSA article, researchers create a handheld laser ophthalmoscope for easy imaging of the retina.
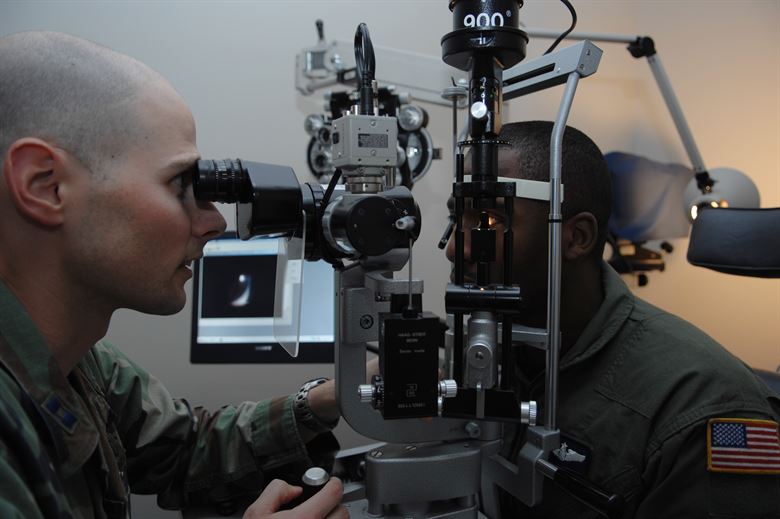
In a standard scanning laser ophthalmoscope the patient head needs to stay still to get a reliable diagnosis. Photo taken by Angelita Lawrence, courtesy of the USAF.
Downsizing of the Setup: Part 1
The wavefront sensor takes up a significant amount of space in a scanning laser ophthalmoscope that utilize adaptive optics. In a conventional ophthalmoscope, the wavefront sensor detects the interference from the eye as the scanner passes over. It then processes the signal which becomes the driver for the deformable mirror to compensate for the eye movements.
Instead of using a physical sensor, the researchers have developed a computational algorithm for on-the-fly deformation. While a conventional wavefront sensing algorithm assumes a single-shot processing, the proposed approach offers a multi-shot computational technique to reliably estimate the wavefront, thus eliminating the need for a physical sensor. A preloaded set of wavefront calculations can help the algorithm to calculate the implied orientation of the eye at any given moment.
Downsizing of the Setup: Part 2
The next step of miniaturization pertains to the adjusting mirror and involves microelectromechanical systems (MEMS). The name is a mouthful, but in this context, it is essentially a mechanically controlled mirror that receives orders from a microprocessor. This connects very small, mechanical instruments with electronic systems so that researchers can manipulate them without manually adjusting the instrument. In this handheld ophthalmoscope, a MEMS enabled deformable mirror is connected and controlled by the wavefront algorithm mentioned before. The algorithm tracks the distortion generated from the eye movement and adjusts the deformable mirror accordingly.
The algorithm accomplishes this by taking a variable mirror shape, instead of holding the shape constant in its calculations. This speeds up the scan time and simplifies the interface with no detriment to the image quality or resolution. The algorithm adjusts the mirror not only for the patient’s eye movements, but also for the doctor’s hand motion.
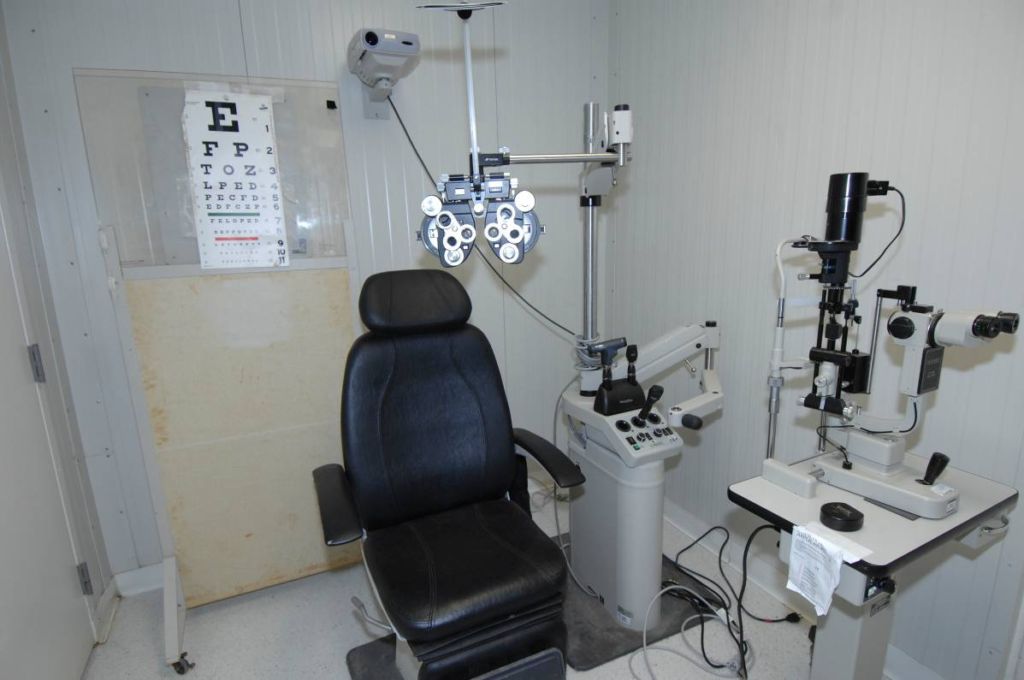
A basic optometry clinic, with bulky examination tools occupying a large space. While rural areas lack access to such clinics, a handheld retinal imaging device such as laser ophthalmoscope can make a huge difference in primary eye care. Photo courtesy of Wikipedia.
Eye Care Problems in Developing Countries
In areas where healthcare is scarce, eye care specialists and technology are luxuries available only to those who can afford private insurance, or high out of pocket expenses. In recent years, emerging countries like Mexico, Argentina, Colombia, Ghana and Nigeria have improved their health insurance systems to subsidize treatment for basic conditions. However, delivering specialized care in an affordable way remains challenging. Places like these administer care through hospitals or primary health care clinics that serve large populations.
Overcrowding is a major issue, while space in these hospitals is often prohibitively expensive. This makes it unaffordable for healthcare providers to dedicate a full room to house one large and cumbersome device, whose strict purpose is an eye examination. Economically speaking, it becomes a poor investment for providers facing a host of primary and urgent care problems. As a result, most retinal disease cases go undetected and untreated leading to high rates of blindness and visual impairment in the least wealthy populations.
Laser Ophthalmoscope for Preventative Care and Pediatrics
A handheld adaptive optics laser ophthalmoscope can bring specialized eye care to the remote locations of our planet. Bringing this technology into primary care facilities can easily eliminate the need to travel far distances to reach a specialized eye care clinic. This can very well become the much needed solution to the preventative care for remote areas as well as for low income people. Even in well developed countries, people under economic stress will often not seek care until a health issue takes clear physical tolls that affect their ability to function. Ironically, the overall lifetime economic cost of an eye care can be so much lower with an early diagnosis.
Moreover, a handheld laser ophthalmoscope can be an ideal tool when dealing with small children an infants or patients who are not fit to sit into the conventional patient chair. It turns out that premature births are vulnerable to retinal disorders as they age. Early diagnostics of any abnormality in such infants will be a major advance in preventative care and could often mean a saved eye. If retinal exams become available to more clinics, including pediatric ones, more preventative measures can be taken to reduce the effects later in life. Overall, it will mean reduced cost for eye care, and less burden to the economy at large.
Further Reading
- Theodore DuBose, Derek Nankivil, Francesco LaRocca, Gar Waterman, Kristen Hagan, James Polans, Brenton Keller, Du Tran-Viet, Lejla Vajzovic, Anthony N. Kuo, Cynthia A. Toth, Joseph A. Izatt, and Sina Farsiu, “Handheld adaptive optics scanning laser ophthalmoscope,” Optica 5, 1027-1036 (2018)
- Hong, H., Mújica, O. J., Anaya, J., Lansingh, V. C., López, E., & Silva, J. C. (2016). The Challenge of Universal Eye Health in Latin America: distributive inequality of ophthalmologists in 14 countries. BMJ Open, 6 (11), e012819. http://doi.org/10.1136/bmjopen-2016-012819
